
2017年1月19日
Salk scientists discover how to prevent undesirable immune attacks on therapeutic viruses
Salk scientists discover how to prevent undesirable immune attacks on therapeutic viruses
LA JOLLA—Normally when we think of viruses, from the common cold to HIV, we want to boost people’s immunity to fight them. But for scientists who develop therapeutic viruses (to, for example, target cancer cells or correct gene deficiencies) a more important question is: How do we keep people’s natural immune responses at bay? In these cases, an overenthusiastic immune response actually undermines the therapy.
Salk Institute researchers discovered that inhibiting a protein called phospholipid scramblase 1 (PLSCR1) controls the infected cell’s antiviral response and provides long-term protection from immune attack and excessive inflammation. The results, described in the January 19, 2017, issue of 神经元, hold promise both for virally delivered treatments and inflammatory conditions like infections; autoimmune disorders such as lupus; or neurodegenerative diseases such as Alzheimer’s disease.
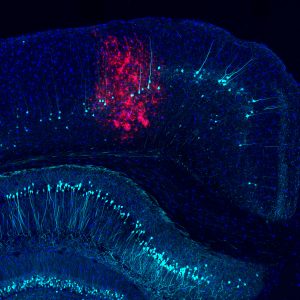
点击此处 用于高分辨率图像
版权:萨克研究所
“Normally, the immune system will quickly recognize and act upon potential threats such as virally infected cells,” says 阿克塞尔·尼默雅恩, assistant professor in Salk’s 韦特先进生物光子学中心 and senior author of the new paper. “But in targeting PLSCR1, we’ve effectively shielded infected cells from immune attack and increased gene expression from an engineered virus from a few days or weeks to at least six months, creating the potential for much longer-lasting therapies.”
Because viruses have evolved such effective methods for finding their target and utilizing the host cells’ own molecular machinery, scientists are modifying viruses into long-lasting therapeutic vehicles that can deliver drugs to specific cells or tissues or selectively target and destroy tumors. But, since our immune systems don’t discriminate between destructive and therapeutic viruses, researchers must devise ways to keep the immune system from destroying the helpful versions.
To better understand the brain’s immune response, the Salk team injected an engineered adenovirus (often used to deliver gene therapy) into mouse brains and monitored both the infected and immune cells’ signaling and protein production in response to infection. Infected cells put out a variety of distress calls, including a molecular flag called phosphatidylserine that summons microglia, specialized immune cells in the brain. Microglia assess the situation and then decide whether to leave the infected cells alone or destroy them. Leaving the distressed cells alone risks having them cause collateral damage to other cells, while destroying them eliminates potentially critical brain cells, many of which don’t regenerate. To better understand the calculus of this decision, the Salk team manipulated levels of the various proteins involved in the cell’s intra- and extracellular communication, including PLSCR1.
Surprisingly, ramping down PLSCR1 caused a wide variety of immune-related changes. Besides keeping microglia at bay, less PLSCR1 resulted in reduced production of inflammatory molecules called cytokines, whose typical role is to recruit more immune cells to the fight. “When we saw how much inhibiting PLSCR1 reduced the inflammatory response, we immediately wondered if this mechanism could apply more broadly, not just to virus infection of the brain, but to other types of infections or even autoimmune diseases,” says Yusuf Tufail, a former Salk postdoctoral fellow and first author of the paper.

点击此处 用于高分辨率图像
版权:萨克研究所
The protective effects of inhibiting PLSCR1 lasted for all time points investigated (up to six months); none of the other manipulated proteins had such a pronounced result. Because PLSCR1 is present throughout the body, not just in the brain, researchers plan to investigate the role of PLSCR1 in other inflammatory conditions.
“Given how complex the immune response is, and how many genes are regulated up or down in response to infection, it was amazing to find a single protein that controls so many pathways,” says Nimmerjahn. “Imagine a small molecule inhibitor that a patient could take to curb excessive inflammation. This could have a hugely beneficial effect on many disease outcomes.”
Other authors included: Daniela Cook, Lawrence Fourgeaud, Colin J. Powers, Katharina Merten, Charles L. Clark, Elizabeth Hoffman, Alexander Ngo, Kohei J. Sekiguchi, Clodagh C. O’Shea, ,和 Greg Lemke of Salk.
The work was funded by grants from the 美国国立卫生研究院; the Rita Allen, Whitehall, Brain Research, Waitt, Hearst, and Richard Allan Barry Family foundations; the Leona M. 和 Harry B. Helmsley 慈善信托基金; the Nomis, H. N. and Frances C. Berger, Fritz B. Burns, and HKT foundations; Frederik Paulsen and Françoise Gilot-Salk; the 国家癌症研究所; the William Scandling Trust; the Price Family Foundation; the Marshall Legacy Foundation; a Life Sciences Research Foundation and Pioneer Fund postdoctoral scholar award; and a Deutsche Forschungsgemeinschaft (DFG) and Catharina Foundation postdoctoral scholar award.
日记
神经元
作者
Yusuf Tufail, Daniela Cook, Lawrence Fourgeaud, Colin J. Powers, Katharina Merten, Charles L. Clark, Elizabeth Hoffman, Alexander Ngo, Kohei J. Sekiguchi, Clodagh C. O’Shea, Greg Lemke, and Axel Nimmerjahn
宣传办公室
电话:(858) 453-4100
press@salk.edu
萨尔克研究所是一个独立的非营利性研究机构,由首个安全有效的脊髓灰质炎疫苗的研发者乔纳斯·索尔克于1960年创立。该研究所的使命是推动以合作、敢于冒险为特点的基础性研究,以应对癌症、阿尔茨海默病和农业脆弱性等社会最紧迫的挑战。这项基础科学支撑着所有的转化研究,产生有助于全球新药和创新的见解。.